Services
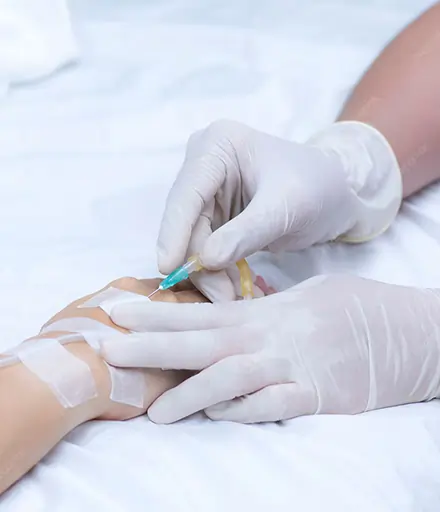
Chemotherapy
Chemotherapy, often simply called "chemo," is one of the most established treatments for cancer, using powerful drugs to target and destroy rapidly dividing cancer cells throughout the body. Imagine it as a systemic "army" that travels via the bloodstream to attack tumors anywhere they hide, whether in the lungs, bones, or brain. Developed in the mid-20th century from wartime research on mustard gas, chemo has evolved dramatically by 2025, saving millions of lives. It's typically administered in cycles—doses followed by recovery periods—to allow healthy cells to rebound. Chemo is versatile: it's used alone or combined with surgery, radiation, or newer therapies. In early-stage cancers like lymphoma, it can cure over 80% of cases; in metastatic disease, it extends survival by months or years. Delivery methods vary—IV infusions in clinics (lasting 30 minutes to days), oral pills at home, or even intraperitoneal washes for ovarian cancer. Modern protocols, guided by guidelines from bodies like the American Society of Clinical Oncology (ASCO), personalize dosing based on body surface area, genetics, and tumor type to minimize harm.
By 2025, supportive care will be so refined that most people will maintain daily activities during treatment. Globally, chemo's role is shifting: it's now a bridge to immunotherapies, reducing tumor burden first. With informed choices and compassionate care, patients navigate it as warriors, emerging stronger.
Targeted Therapy
Targeted therapy represents a revolutionary shift in cancer care, honing in on specific molecular "Achilles' heels" of tumors rather than blasting everything in sight like traditional chemo. By 2025, these drugs will act like smart missiles, binding to proteins or genes that cancer cells over-rely on for survival, sparing most healthy cells and reducing side effects. For everyday folks, targeted therapies shine in cancers with identifiable drivers—think HER2-positive breast cancer, where trastuzumab (Herceptin) tags the rogue protein for immune destruction, boosting cure rates from 75% to 90%. Or EGFR-mutated lung cancer, where osimertinib halts growth signals, extending life by 18 months on average. Development exploded post-2000s genome sequencing; now, over 100 FDA-approved agents target pathways like VEGF (for angiogenesis in kidney cancer) or BRAF (in melanoma). Oral pills like these allow home treatment, freeing patients from clinic IVs.
How do we know it fits? Biomarker testing—simple blood or tissue samples—guides selection. In precision medicine hubs, next-generation sequencing (NGS) scans for mutations in days. Real-world impact: A farmer with colorectal cancer, KRAS wild-type, thrives on cetuximab, avoiding surgery. As genomics democratizes, targeted therapy isn't elite—it's the new standard, turning "one-size-fits-all" medicine into tailored triumphs, fostering hope in the cancer journey.
Book your appointment with Dr. Dhruv Mehta today!
Call: +91 932 7719 032Book an Appointment
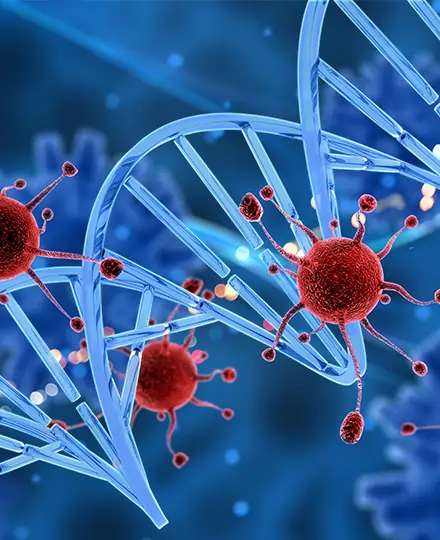
Immunotherapy
Immunotherapy, the "holy grail" of modern oncology, turbocharges the immune system to recognize and obliterate cancer cells that normally hide like stealth invaders. Unlike chemo's blunt force, it unleashes natural killers like T cells and NK cells. By November 2025, it's transformed "incurable" cancers: melanoma survival leaped from 25% to 55% five-year rates, and lung cancer patients live years longer. For the public, grasp this: Our immune system patrols constantly but falters against cancer's camouflage (e.g., PD-L1 shields). Immuno drugs, often IV every few weeks, retrain it CAR-T cells, engineered from a patient's blood, hunt blood cancers with 80% remission in refractory lymphomas. Vaccine-like approaches, such as Sipuleucel-T for prostate cancer, prime responses. It's game-changing for 20-30% of responders, especially in MSI-high tumors across types. Side effects differ—autoimmune flares like colitis or thyroid issues (10-20% severe, treatable with steroids)—but there is no hair loss or sterility like with chemo.
Challenges? Not universal—cold tumors (low mutation burden) resist, sparking combos with radiation to "heat" them up. Cost barriers persist (4.5 to 6 lakhs yearly), though India's biosimilars and trials democratize access. Ultimately, immunotherapy isn't just treatment—it's a partnership with biology, evoking awe at our inner warriors. As research unmasks more evasion tactics, it promises broader cures, turning despair into durable victories for families worldwide.
Hormone Therapy
Hormone therapy, or endocrine therapy, is a gentle yet potent weapon against cancers driven by sex hormones like estrogen or testosterone, which act as fertilizers for tumor growth. Primarily for breast and prostate cancers—80% hormone-sensitive—it's like turning off the tap: drugs block production or action, starving cells. Tamoxifen, a pioneer since the 1970s, revolutionized breast cancer, slashing recurrence 50% in premenopausal women by binding estrogen receptors. By 2025, refinements abound: CDK4/6 inhibitors (palbociclib) added to hormone drugs boost progression-free survival to 28 months in advanced breast cancer. Side effects? Hot flashes, bone thinning (countered by bisphosphonates), or fatigue—but far milder than chemo, allowing work and hobbies. In diverse settings like India, where breast cancer hits 200,000 women yearly, affordable tamoxifen generics empower rural access.


Palliative Care
Palliative care focuses on comfort, not cure—relieving suffering from cancer and its treatments, from diagnosis onward. WHO defines it as improving life for serious illnesses; for cancer, it manages symptoms in 70% of patients, extending quality months. Benefits: Better sleep and mood; families report less burnout. Myths: "Weakens fight"—evidence shows the opposite, enabling tolerance for aggressive therapy. Palliative care isn't giving up; it's gearing up for better days amid cancer's toll. From chemo fatigue to tumor pain, it tailors relief.
Pain Management
Cancer pain affects 60-80% of patients, from bone metastasis to nerve compression, but it's treatable in 90% of cases. Management follows the WHO ladder: Step 1, non-opioids (paracetamol); Step 2, weak opioids (codeine); and Step 3, strong opioids (morphine). Pain isn't "tough it out"—it's a signal needing to be addressed, improving appetite and sleep. Opioid fear? Addiction is rare (<1% cancer); rotation prevents tolerance. Nerve blocks for neuropathic pain and radiotherapy for bone pain are further options for cancer pain relief.


Precision Oncology
Precision oncology tailors treatment to your tumor's genetic blueprint, using NGS to spot mutations like BRCA in breast or KRAS in colon. From the 2010s boom, 2025 sees 60% of advanced patients benefit, with matched therapies doubling responses. Process: Biopsy → sequencing (₹20,000-50,000) → match drugs (e.g., PARP inhibitors for BRCA). Benefits: Avoids ineffective chemo, reduces toxicity. Challenges: cost and access. Myths: "Only the rich" can afford generics. Its future: From off-label to trials. Empower yourself: Ask for a profiling from your oncologist. Precision turns one-size-fits-all into you-fit-best.
Screening and preventive oncology
Screening detects precancers early—mammograms for breast cancer (done at age 40+), colonoscopies for colorectal cancer (for ages 45+), and Pap smears and co-testing for cervical cancer. Prevention—vaccines (the HPV vaccine cuts 90% of cervical cancer incidence) and lifestyle modifications (no smoking, plenty of fruits and veggies, and exercise). Benefits—50% mortality drop. "Myths—'Overdiagnosis'—Appropriate interpretation of screening tests balances risks. In 2025, AI reads scans 95% accurately. Community camps boost uptake. Prevention—Aspirin for the prevention of colon cancer in high-risk cases. Knowledge saves—screen, vaccinate, thrive.


Pathology lab
Oncopathology examines tissues to identify cancer type, grade, local invasion, and size via biopsies, immunohistochemistry, and FISH tests. Pathologists are detectives—microscopes reveal cell chaos; molecular tests spot targets. The process involves obtaining a tissue sample → stain → report (in 7-10 days). Digital pathology speeds 2025 reads. Challenges include shortages in rural India—telepathology helps. Advances in oncopathology—AI (artificial intelligence) assists, reducing errors in 20% of cases. From frozen sections in surgery to NGS integration, oncopathology is a detective behind every cancer diagnosis. Appreciate your pathologist, as a good pathology report unlocks your therapeutic armamentarium. It's quiet heroism in oncology's frontline war.
