Kidney & ovarian cancer specialists recommend people look out for the following symptoms-
- Constant Urination.
- Blood In Urine.
- Pelvic Discomfort.
- Lower Back Pain.
- Swelling In Legs.
For Women-
- Abnormal Vaginal Bleeding.
- Swelling In Lower Abdomen.
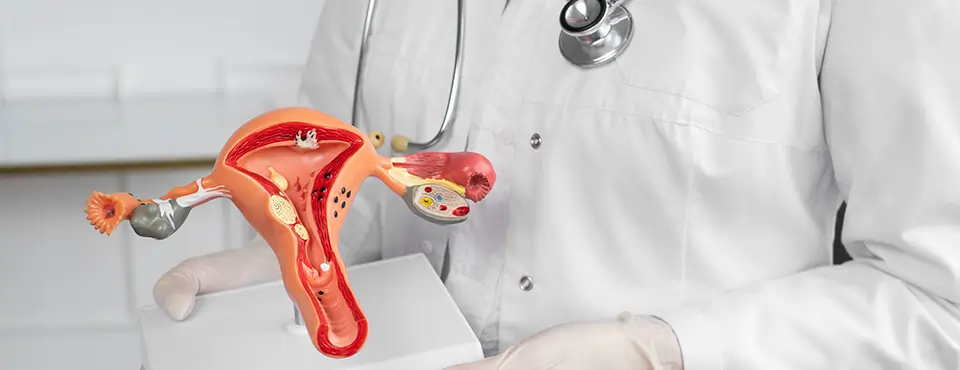
Genitourinary (GU) cancers refer to cancers that affect the organs involved in urine production, storage, and expulsion, as well as the male reproductive system. The term "genitourinary" combines "genital" (reproductive organs) and "urinary" (kidney, bladder, and urethra). These cancers are common worldwide and can significantly impact quality of life, but early detection and modern treatments from a kidney cancer specialist or an ovarian cancer specialist offer hope for many patients. The main types of GU cancers include kidney cancer, bladder cancer, prostate cancer (almost exclusively in men), testicular cancer (primarily in younger men), and penile cancer. In India, GU cancers are a growing concern due to an aging population, lifestyle changes, and environmental factors.
Kidney cancer (renal cell carcinoma), about 2-3% of all adult cancers in India, is more common in northern India (Punjab, Haryana) than in the south. Smoking, obesity, high blood pressure, and long-term painkiller use are major risks. Bladder cancer is strongly linked to tobacco use—smoking increases risk 4-fold, and chewing tobacco (common in India) adds to the danger. Industrial chemicals (dyes and paints) affect workers in textile and leather industries, especially in Gujarat and Tamil Nadu. Prostate cancer incidence has increased by 2-3% annually over the last two decades. Risk factors include older age (most cases after 65), family history, and diets high in red meat and dairy. Indian men often present at later stages because screening is not routine. Testicular cancer is rare, and it affects young men (15-35 years). Undescended testes (cryptorchidism) increase risk 4-8 times. Survival is excellent (>95%) with early treatment from a kidney cancer specialist. Penile cancer is very rare globally, but in India its incidence is higher in rural areas. Poor hygiene, lack of circumcision, and human papillomavirus (HPV) infection are key risk factors.
Symptoms vary by cancer type and stage. Many GU cancers are "silent" in early stages, which is why awareness guided by a kidney cancer specialist is crucial.
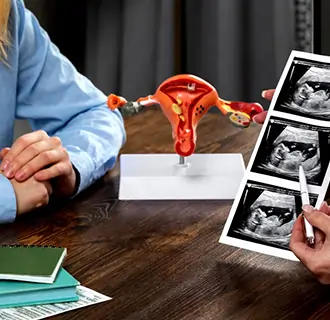
Diagnosis done by a kidney cancer specialist combines history, physical exam, blood/urine tests, imaging, and biopsy. Blood tests include PSA for prostate (normal <4 ng/mL), serum creatinine for kidney function, and complete blood count (CBC) for anemia. Urinalysis for blood/protein and urine cytology (looks for cancer cells—useful in bladder) are urine tests done for GU cancer detection. Imaging tests depend on the site of the cancer and include CECT, MRI, and PET-CT. Biopsy is required for definitive diagnosis. The method for biopsy is different for each site and is as follows:
With the help of all the above investigations, TNM staging is done, and further management is decided.
Treatment of any cancer depends on cancer type, stage, patient age, and comorbidities.
With the advancement of molecular tests, any advanced cancers can be analyzed by an ovarian cancer specialist for mutations that can be targeted with newer available therapies for personalized and precision care.
After completion of therapy from an ovarian cancer specialist, long-term follow-up is required to detect recurrences and second primary cancers and to look for late toxicities of chemotherapy and radiation. It is important to watch for symptoms that could signal the return of cancer—headaches, convulsions, shortness of breath, chronic cough, bony pains, abdominal pain or distension, jaundice, weight loss despite adequate food intake, etc. The general schedule for checkups is 3 monthly in the first 2 years, 6 monthly between years 3 and 5, and annually after 5 years. Check-ups specific to the site would be advised by the treating ovarian cancer specialist. Also, lifestyle modifications like quitting tobacco/alcohol, maintaining a healthy weight (BMI < 25), exercising 150 min/week, eating plenty of fruits and vegetables, and limiting red meat are advised. The HPV vaccine (preferably Gardasil 9) for boys and girls between ages 9 and 26 years prevents penile and cervical cancer.
In India, rising incidence demands proactive screening—PSA after 50 (high-risk after 40), urine checks for smokers, and self-exams for testicular lumps. If you or a loved one faces symptoms, consult an oncologist. Early-stage cure rates exceed 90% for most GU cancers. Knowledge empowers—share this information to save lives.
Kidney & ovarian cancer specialists recommend people look out for the following symptoms-
For Women-
Genitourinary cancers are cancers of the urinary & reproductive systems. Kidney & ovarian cancer specialists categorize if it happens in any of these organs-
An ovarian & kidney cancer specialist often starts by asking about your health, heredity, & doing a physical checkup. After that, he runs the following tests to check for cancer-
Based on the type of cancer that a patient has, the spread in the body, & overall health, an ovarian & kidney cancer specialist decides from-